The author developed his GH-Method: math-physical medicine (MPM) by applying mathematics, physics, engineering modeling, and computer science (big data analytics and AI) to derive the mathematical metabolism model and three prediction tools for weight, FPG, and PPG with >30 input elements. This study includes 11 categories: weight, glucose, blood pressure, lipids, food, water, exercise, sleep, stress, life pattern regularity, time with ~500 input and output elements. He collected more than 1 million “clean” data over 7 years.
Type 2 diabetes, cardiovascular risk, obesity, metabolism, metabolic conditions, chronic diseases, lifestyle data, artificial intelligence and math-physical medicine.
By using the GH-Method: math-physical medicine and big data on one particular patient (the author), this clinical paper utilized the results to describe the relationship between his metabolic state and medical conditions, including obesity, type 2 diabetes (T2D), and cardiovascular risk [1].
The obese patient was diagnosed with T2D, hyperlipidemia, and hypertension over 25 years ago and suffered five cardiac episodes during 1994-2006. For this study, approximately 1.5M detailed metabolic conditions and lifestyle data (1/1/2012 - 12/31/2018) were collected and processed; advanced mathematics, physics concepts, engineering modeling, and artificial intelligence (AI) were utilized rather than following the traditional biology and chemistry approach as research tools. The author defined two new terms: Metabolism Index (MI) and General Health Status Unit (GHSU) to evaluate his overall metabolism and associated chronic diseases [2].
Here Are the Steps to His Research Process
1. Observing physical phenomena and metabolic changes, collecting relevant data using software;
2. Applying appropriate engineering modeling and deriving various inter-relationship mathematical equations for predictions, along with applying statistics tools for variance and sensitivity studies.
3. Using machine learning and AI to predict important metabolic changes [3].
Table 1. Chronic Diseases, Including Obesity, T2D, Hyperlipidemia, Hypertension Show Significant Improvements When Metabolism Improved
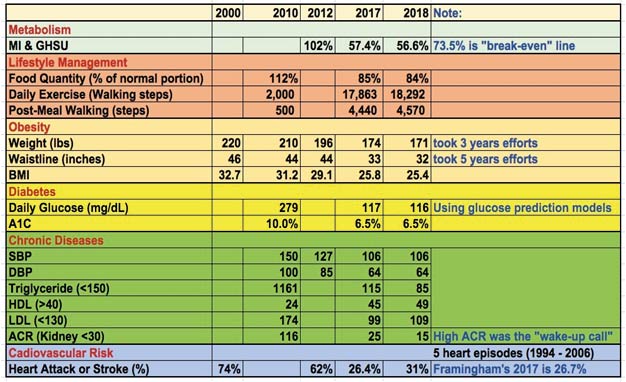
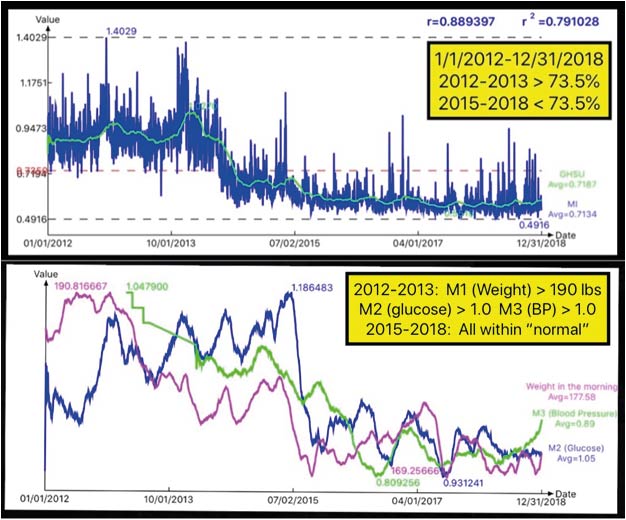
Figure 1. Relationship between Metabolism, Including MI, GHSU and Chronic Diseases
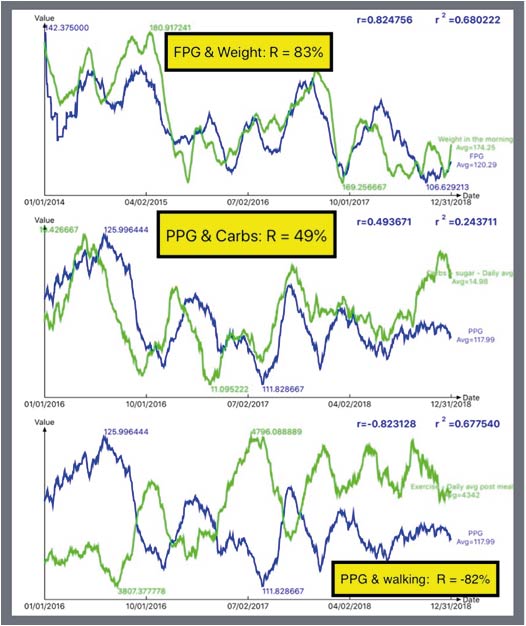
Figure 2. Relationship between T2D and Weight, Food, and Exercise
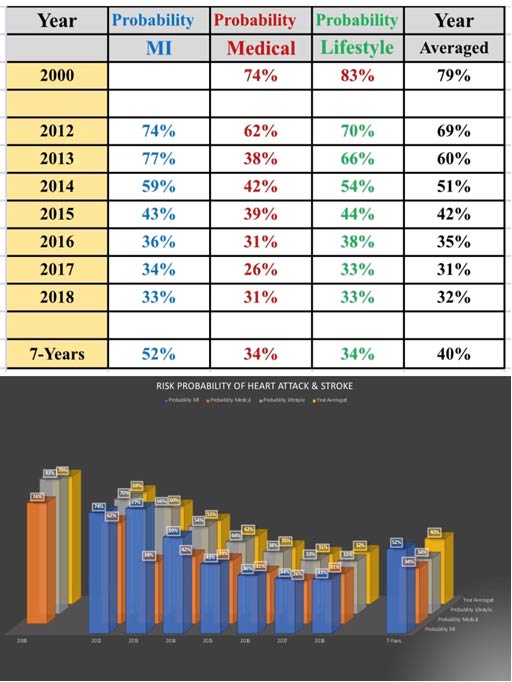
Figure 3. Risk Probability of Having a Heart Attack or Stroke Dropping Significantly
Table 1 displays some of his key metabolic factors and health symptoms within nine years (2010-2018).
Figure 1 shows the close relationships existing between Metabolism, including MI, GHSU, and chronic diseases (2012-2018).
Figure 2 demonstrates the various degrees of correlations between T2D conditions and influential factors: weight, food, and exercise (2016-2018).
Figure 3 illustrates the risk probability of having a heart attack (CVD) or stroke dropping significantly (2010-2017).
This math-physical medicine approach has quantitatively proven the close relationship between metabolic changes due to lifestyle improvement and effective chronic disease control [4].
- Hsu Gerald C (2018) Using Math-Physical Medicine to Control T2D via Metabolism Monitoring and Glucose Predictions. Adv Endo and Dia 1: 1-6. [Crossref]
- Hsu Gerald C (2018) Using Signal Processing Techniques to Predict PPG for T2D. Int J Diabetes Metab Disord 3: 1-3. [Crossref]
- Hsu Gerald C (2018) Using Math-Physical Medicine and Artificial Intelligence Technology to Manage Lifestyle and Control Metabolic Conditions of T2D. Diabetes Complications 2: 1-7. [Crossref]
- Hsu Gerald C (2018) Using Math-Physical Medicine to Study the Risk Probability of having a Heart Attack or Stroke Based on Three Approaches, Medical Conditions, Lifestyle Management Details, and Metabolic Index. EC Cardiology 5: 1-9. [Crossref]




