The association of Langerhans Histiocytosis and solid neoplasia or hemopathies has been described in several studies. Nevertheless, the occurence of germinal cell tumor is rarely reported. Herein we report the case of 28-year-old patient who was referred to internal medicine for suspicion of Langerhans histiocytosis. The patient was diagnosed with germinal tumor of testicle and had a left orchi - epididymectomy. In the assessment of tumor extension, kystic pulmonary lesions were diagnosed suggesting Langerhans histiocytosis. The diagnosis was confirmed with the broncho-alveolar lavage which recovered macrophagic alveolitis with CD1a positive in 10% of macrophages. Investigations concluded to non-progressive disease and therapeutic abstention and surveillance was decided. The present case is another exceptional co-association of Langerhans Histiocytosis and germinal cell tumor. It suggests that the simultaneous association is due to a possible genetic process.
Langerhans Cell Histiocytosis (LCH) is a rare disease of young adult males. The clinical manifestations are quite polymorphous and the prognosis is very varied [1,2]. The combination of LCH and neoplasia has been described in several studies mainly in pediatric series. We report the case of an adult patient presenting a pulmonary LCH associated with a mixed germinal sub capsular tumor of the left testis.
A 28-year-old patient smoking with 10 packets / year was referred to internal medicine for suspicion of Langerhans's histiocytosis. The patient was hospitalized in March 2013, at the Urology Department, for a painful left inguinal swelling. Testicular ultrasound showed an atrophic right testicle in place with epididymis of normal appearance. The left testis is of inguinal seat with pseudo-nodular heterogeneous hypertrophied aspect and a fuzzy limits containing areas of necrosis and calcifications. The left epididymis is thickened heterogeneous and contains calcifications. This echographic pattern was quite suggestive of a malignancy. The serum determination of tumor markers was within normal: a level of LDH at 220 U / l (<1, 5XN), an α feto -protein level at 85 ng / ml (<100ng/ml) and beta HCG at 5ng / ml (<5000ng/ml). The patient had a left orchi - epididymectomy. The histopathological examination of the surgical specimen found a sub capsular mixed germinal tumor of the testicle with extensive necrotic foci and without epididymal infiltration. (Figure 1)
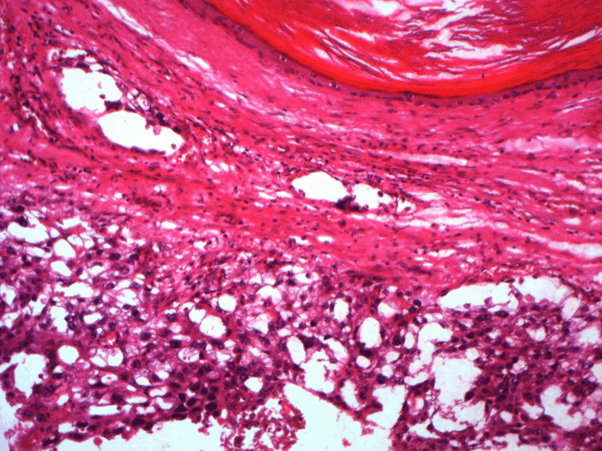
Figure 1. Teratoma component of germinal cell tumor (HEx400)
The thoraco-abdominopelvic scanner revealed a retro-peritoneal adenomegaly and multiple cystic lesions of millimeter size disseminated in the lung fields, sparing the basics suggestive of LCH. The patient was treated with 3 cures of Bleomycin - Etoposide - Cisplatin. The bronchoalvelar lavage recovered macrophagic alveolitis with CD1a positive in 10% of macrophages. Then, the patient was referred to internal medicine for assessment of his illness and therapeutic decision. Biological assessment including inflammatory markers, renal and hepatic tests were strictly normal. The chest scan tomography performed after three months of diagnosis showed multiple scattered millimetric bubbles in both lung fields of non-progressive appearance. The bone scintigraphy was without abnormalities. After these explorations, the diagnosis of non-progressive infra-clinical pulmonary LCH was retained. Therapeutic abstention and surveillance was decided.
LCH is a rare disorder of histiocyte proliferation. Previous case studies suggest a higher prevalence of hematologic and solid malignancies among LCH patients [3]. This association was explained by tumorigenic agents such as etoposide widely used in the treatment of LCH. In the present case we report a rare association of LCH and germ cell tumor. The diagnosis of both disease was concomitant suggesting another pathogenic pathway [4]. In this contest, the discovery of the prevalence of BRAF/ERK pathway mutations in LCH, observed in almost 50% of cases, may be a risk factor for the increased rate of malignancies mainly the hemopathies [5]. This gene plays an important role in cell cycle regulation and in proliferartion. In the review of literature of 93 cases of neoplasias including leukemias, Hodgkin and non-Hodgkin lymphomas and soft tissue tumors, Egeler did not find any cases of LCH coincident with germ cell tumor [4]. In a recent large study of prevalence of neoplasm in 132 adult’s patients, 42 (32%) patients had an additional malignancy [3]. Solid tumors were the most prevalent, none of them was germinal cell tumor [3]. The first cases of simultanely occurring of systemic LCH and mediastinal germ cell tumor were reported 1988 [6]. Then, few cases of germinal cell tumor and LCH have been reported [7-11] (Table1). Malgorzata, reported this association in 2-year-old girl, in whom two foci of LCH in the left parietal bone and right humerus were diagnosed 5 months after completion of chemotherapy with etoposide, ifosfamide and cisplatin. No relapses of either disease have been observed within 24 months after the completion of treatment [10]. In this contest, new therapeutic strategies of testicular germinal tumor have established. For stage I seminomatous germ cell tumours, the choice is between monitoring, chemotherapy (1 carboplatin cycle) or para-aortic radiotherapy. Treatment for stage I non seminomatous germ cell tumours is based on surveillance, chemotherapy (1 cycle of Bleomycine, etoposide and cisplain) or staging retroperitoneal lymphadenectomy. The management of metastatic tumours consists of chemotherapy with 3, 4 cycles of BEP or dose-dense chemotherapy. Radiotherapy is indicated in seminomas with lymph node metastasis. Surgical retroperitoneal lymph node dissection is indicated for all residual non-seminomatous germ cell tumour masses > 1 cm and for persistent residual seminoma masses > 3 cm with 18-fluoro-desoxy-glucose PET- CT uptake [12]. Through the reported cases, the prognosis of the association depends on the form of LCH and the involvement of risk organ [13]. In conclusion, LCH may be diagnosed stimulanely or before the malignant disease suggesting a cause of malignancy independent of LCH treatment. Several type of neoplasms have been reported. Germinal tumor as in our patient are exceptional. Therefore, the diagnosis of solid tumors should be kept in mind during the course of LCH. Further exploration of the genetic and biology of LCH and its underlying processes is warranted to elucidate the mechanisms of increased association of malignancies and even the type of neoplasm in adult and pediatric patients with LCH.
Table 1: Review of literature of the association between germinal cell tumor and LH.
N° Case |
1(6) |
2 (7) |
3 (8) |
4 (9) |
5 (10) |
6 (11) |
Age |
33 |
35 |
22 |
18 |
2 |
35 |
Sex |
M |
F |
M |
M |
F |
H |
Date of onset of germinal cell tumor |
Post mortem
(after diagnosis of LCH) |
25 years before
LCH |
Simultanely
With LCH |
Simultanely
With LCH |
5 months before
LCH |
5
months before
LCH |
Location of germinal cell tumor |
Mediastin |
Ovary |
Mediastin |
Testis |
Buttock |
Testis |
Form of LCH |
Diffuse LCH |
Bone LCH
(clavicale) |
Diffuse LCH |
Diffuse LCH |
Bone
LCH
(parietal and humerus bone) |
Pulmonary
LCH |
Type of treatment of LCH |
- |
Surgical |
Chemotherapy |
Aggressive chemotherapy |
Surgical |
- |
Outcome LCH/germinal cell tumor |
Death |
No relapse of germinal cell tumor
and LCH |
Death |
Death |
No relapses of germinal cell tumor and LCH |
No relapses of germinal
cell tumor |
- Stéphan JL (2002) Histiocytoses langerhansiennes et non langerhansiennes. Arch Pediatr. 9: 934-941. [Crossref]
- Nguyen K, Tazi A (2006) Histiocytose Langerhansienne de l’adulte. Le revue de praticien. 56: 1863-1871. [Crossref]
- Ma J, Laird JH, Chau KW, Chelius MR, Lok BH, et al. (2019) Langerhans cell histiocytosis in adults is associated with a high prevalence of hematologic and solid malignancies. Cancer Med. 8: 58-66. [Crossref]
- Elegar RM, Neglio JP, Puccetti DM, Brennan CA, Nesbit ME (1993) Association of Langerhans’ cell histiocytosis with malignant neoplasms. Cancer. 71: 865-873. [Crossref]
- Badalian‐Very G, Vergilio JA, Degar BA, MacConaill LE, Brandner B, et al. (2010) Recurrent BRAF mutations in Langerhans cell histiocytosis. Blood. 116: 1919‐1923. [Crossref]
- Ladanyi M, Roy I (1988) Mediastinal germ cell tumors and histiocytosis. Hum Pathol. 19: 586-590. [Crossref]
- Margolin K, Traweek T (1992) The unique association of malignant histiocytosis and primary gonadal germ cell tumor. Med Pediatr Oncol 20: 162-164. [Crossref]
- Takahashi S, Asamoto M, Nakazawa T, Kosaki T, Katsumi K, et al. (1994) Robb-Smith type malignant histiocytosis associated with a mediastinal germ cell tumor. Jpn J Clin Onc. 24: 327-330. [Crossref]
- Ng WK, Lam KY, Ng IO (1995) Langerhans cell histiocytosis: possible association with malignant germ cell tumour. J Clin Pathol 48: 963-965. [Crossref]
- Szumera M, Popadiuk S, Borkowska A, Korzon M (2003) Association of germ cell tumor and Langerhans histiocytosis in a 2-year old child. Case Rep Clin Pract Rev. 4: 107-110. [Crossref]
- Nikolaos P, Adamantia N, Maria R, Aggelos E, Spryridon M, et al. (2015) Langerhans cell histiocytosis following treatment for testicular cancer. A case report and literature review. HeSMO. 6: 6-9. [Crossref]
- Durand X, Fléchon A, Murez T, Rocher L, Camparo P, et al. (2016) CCAFU french national guidelines 2016-2018 on testicular germ cell tumors. Prog Urol. 27: S147-S166. [Crossref]
- Grana N (2014) Langerhans Cell Histiocytosis. Cancer Control. 21: 328-334. [Crossref]

