Although clinical symptomatology and electrocardiogram (ECG) findings of acute pericarditis have been well described, the diagnosis can still be perplexing in some instances. We report here a case of early acute pericarditis which was taken to the cardiac catheterization lab for coronary angiography with suspected acute myocardial infarction (MI). The ECG initially showed regional ST elevation, but later became diffuse. The case demonstrates that in the earliest phase of pericarditis, ST-elevations may be regional, making it difficult to distinguish from an acute MI. We present the ECG recordings which show this progression. Other factors which may help in differentiating pericarditis from acute MI are also discussed.
acute pericarditis, ST-elevation, myocardial infarction
Presenting features of acute pericarditis include chest pain, pericardial friction rub, classic ECG changes, and an inflammatory pericardial effusion on echocardiography. Widely accepted diagnostic criteria only require two of the four mentioned characteristics for diagnosis. Classic ECG changes are described in four stages; (Stage 1) diffuse ST-elevation with PR-depression, (Stage 2) return of ST and PR segment to isoelectric baseline, (Stage 3) T-wave inversion, and (Stage 4) gradual resolution of ECG changes [1-2]. Unfortunately, many patients with pericarditis are initially diagnosed as acute MI and taken to the cardiac catheterization laboratory for coronary angiography, exposing them to unnecessary risk [3]. We present here a patient with early acute pericarditis originally diagnosed as an acute inferior MI. The ECG recordings initially showed regional ST elevation, but later became diffuse. Our case demonstrates that in the earliest phase of pericarditis the ST-elevations may be regional making it difficult to distinguish from acute MI. Other considerations may also assist in differentiating the two conditions.
A cardiology consultation was requested for a 56 year old man in the intensive care unit who was complaining of chest pain. The patient had been admitted 3 days prior with a diagnosis of spontaneous right-sided pneumothorax which was resolving. The chest pain was located in the mid chest and described as dull. The pain worsened with deep inspiration, but was not associated with any other symptoms.
Examination of the patient revealed a blood pressure of 132/76 mm Hg and a pulse rate of 125 beats per minute. He was afebrile. The cardiac rhythm was irregular with varying intensity of the first heart sound. Lung sounds were diminished on the right side, and respiratory effort seemed decreased. The remainder of the physical exam was unremarkable.
ECG showed atrial fibrillation with rapid ventricular response at a rate of 139 beats per minute (Figure 1). ST segment elevation was noted in leads II, III and aVF suggestive of acute inferior MI. The patent was taken emergently for cardiac catheterization, which revealed normal coronary arteries and left ventricular systolic function. ECG performed after cardiac catheterization showed diffuse ST segment elevation involving the anterolateral and inferior leads with diffuse PR segment depression consistent with the diagnosis of pericarditis (Figure 2). Follow up 2-dimensional transthoracic echocardiography (2D-TTE) showed a left ventricular ejection fraction of 55-60% and a small pericardial effusion.
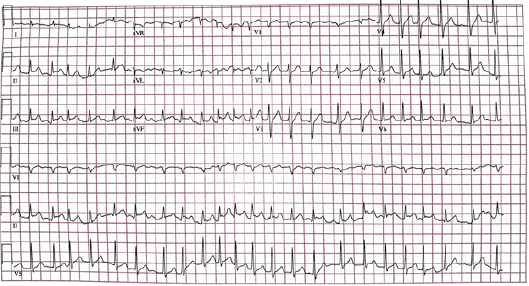
Figure 1: ECG showing atrial fibrillation with rapid ventricular response at a rate of 139 beats per minute and regional ST segment elevation in the inferior leads, suggestive of acute inferior myocardial infarction.

Figure 2: ECG showing sinus tachycardia at a rate of 107 beats per minute, diffuse ST segment elevation involving the anterolateral and inferior leads and diffuse PR segment depression consistent with pericarditis.
Treatment was initiated with colchicine 0.5 mg twice daily for three months. Immediate clinical improvement was noted with complete resolution of chest pain and ECG normalization over the next 48 hours.
It is estimated that up to five percent of emergency department visits for chest pain may be related to pericarditis [4]. Clinically, acute pericarditis can mimic acute MI with similar symptoms, ECG and exam findings. Even the classic pericardial friction rub associated with pericarditis may be encountered after MI, although usually late in the presentation. It is therefore crucial to take the entire clinical picture into consideration, including aggravating and alleviating factors, risk factors, and timing of ECG changes, when diagnosing pericarditis. The four stages of pericarditis can be determined by ECG; These changes include diffuse, upward concave ST-segment elevation, T-wave inversion, and PR-segment depression. The progression of these phases can be a distinguishing factor that helps differentiate pericarditis from acute MI and early repolarization [4]. Stage one can last hours to days and involves ST segment elevation with T waves remaining upright, and PR segments becoming isoelectric or depressed. Eventually, the ST and PR segments return to baseline which signifies transition into stage two. Stage three involves diffuse T-wave inversion, which remain after the ST segments have normalized. The ECG returns to baseline in stage four with the exception of progression to chronic pericarditis, which is reflected in the persistence of T-wave inversion [4-5].
In order to differentiate pericarditis from acute MI, other determining aspects of the clinical presentation and ECG may be considered. Spodick’s sign, the downslope of the T-P segment, has previously been described as a sign of pericarditis. A retrospective study proved that although Spodick’s sign was statistically significant for pericarditis, it was also seen in 5% with acute ST-elevation MI [6]. Some clinicians described the presence of ST-depression in lead aVL as highly sensitive for coronary occlusion and not in pericarditis [7]. Another study noted that acute pericarditis does not manifest prolongation of the QRS complex and shortening of the QT interval, which is frequently seen in acute infarction [8]. Additional ECG manifestations which are more suggestive of MI include the presence of Q waves and loss of R-wave voltage [5]. Another important finding in the diagnosis of acute MI is the presence of ST segment depression in the reciprocal leads. The presence of atrial fibrillation was also found to be uncommon in acute pericarditis in the absence of underlying heart disease. Atrioventricular blocks, ventricular arrhythmias, and atrial fibrillation were all more common in the setting of acute MI [9-11].
It should also be noted that in addition to acute MI, ST-elevations that mimic pericarditis, have also been reported in gastrointestinal disorders, including pancreatitis, hepatitis, peritonitis, and intestinal perforation [1]. Monti et al have presented a unique case of Brugada syndrome mimicking acute pericarditis [12]. A few cases of regional pericarditis with regional ST elevation have also been reported [13-16]. It is crucial that clinicians distinguish pericarditis from acute MI since the management of the two conditions is so markedly different. [17].
Our case demonstrates that at the very onset, acute pericarditis may present with regional ST-elevation, problematically mimicking acute MI. It is especially important to make every attempt to differentiate pericarditis from acute MI, as anticoagulants, platelet inhibitors and thrombolytics used for the treatment of MI may worsen acute pericarditis.
None
None
- Youssef, G., Khouzam, S., Sprung, J., & Bourke, D. L. (2001). Regional pericarditis mimicking myocardial infarction. The Journal of the American Society of Anesthesiologists, 95(1), 261-264.
- Masek, K. P., & Levis, J. T. (2013). ECG diagnosis: acute pericarditis. The Permanente Journal, 17(4), e146.
- McCORD, M. C., & TAGUCHI, J. T. (1951). Nonspecific pericarditis: a fatal case. AMA archives of internal medicine, 87(5), 727-731.
- Tingle, L. E., Molina, D., & Calvert, C. (2007). Acute pericarditis. American family physician, 76(10), 1509-1514.
- Snyder, M. J., Bepko, J., & White, M. (2014). Acute pericarditis: diagnosis and management. American family physician, 89(7), 553-560.
- Witting, M. D., Hu, K. M., Westreich, A. A., Tewelde, S., Farzad, A., & Mattu, A. (2020). Evaluation of Spodick's Sign and Other Electrocardiographic Findings as Indicators of STEMI and Pericarditis. The Journal of emergency medicine, 58(4), 562-569.
- Bischof, J. E., Worrall, C., Thompson, P., Marti, D., & Smith, S. W. (2016). ST depression in lead aVL differentiates inferior ST-elevation myocardial infarction from pericarditis. The American journal of emergency medicine, 34(2), 149-154.
- Rossello, X., Wiegerinck, R. F., Alguersuari, J., Bardají, A., Worner, F., Sutil, M., ... & Cinca, J. (2014). New electrocardiographic criteria to differentiate acute pericarditis and myocardial infarction. The American journal of medicine, 127(3), 233-239.
- Ariyarajah, V., & Spodick, D. H. (2007). Acute pericarditis: diagnostic cues and common electrocardiographic manifestations. Cardiology in review, 15(1), 24-30.
- Lange, R. A., & Hillis, L. D. (2004). Acute pericarditis. New England Journal of Medicine, 351(21), 2195-2202.
- Marinella, M. A. (1998). Electrocardiographic manifestations and differential diagnosis of acute pericarditis. American family physician, 57(4), 699.
- Monti, M., Olivi, G., Francavilla, F., & Borgognoni, F. (2017). Pericarditis mimicking Brugada syndrome. The American journal of emergency medicine, 35(4), 669-e1.
- Jain, A. (1997). “Tombstone” anterior st‐segment elevations secondary to acute pericarditis: the role of two‐dimensional echocardiogram. Clinical cardiology, 20(4), 404-406.
- Oliva, P. B., Hammill, S. C., & Edwards, W. D. (1993). The electrocardiographic diagnosis of regional pericarditis in acute inferior myocardial infarction. European heart journal, 14(12), 1683-1691.
- Dorfman, T. A., & Aqel, R. (2009). Regional pericarditis: a review of the pericardial manifestations of acute myocardial infarction. Clinical Cardiology: An International Indexed and Peer‐Reviewed Journal for Advances in the Treatment of Cardiovascular Disease, 32(3), 115-120.
- Chhabra, L., & Spodick, D. H. (2014). Electrocardiography in pericarditis and ST-elevation myocardial infarction: timing of observation is critical. The American journal of medicine, 127(5), e17.
- Goyle, K. K., & Walling, A. (2002). Diagnosing pericarditis. American family physician, 66(9), 1695.


